Three years ago, a sudden fever struck veteran science writer Brian Vastag on a blue-sky Wisconsin morning. He’s been sick ever since. Now cognitively and physically disabled, he lives on the island of Kauai. On Brian’s third “illiversary,” he presents an opportunity to National Institutes of Health Director Francis Collins.
Dear Dr. Collins,
You might recall the last time we spoke. It was January 2013, and I was working as a science reporter at The Washington Post. Your people arranged an early call for you to announce that the N.I.H. had decided to retire most of its research chimpanzees. We spoke for about 20 minutes, and I typed up a 600-word story. It wasn’t very good.
I was working from home that gray day because I had little choice. I was mostly bedbound then, seven months after a sudden fever had knocked me prostrate. My legs were so weak that climbing the stairs to my home office required pulling myself up the railing hand-over-hand. My brain was so sluggish I asked few questions of you. The ones I managed to croak out were poor, no doubt.
Too sick to work, I did anyway. I loved my job at the Post – not an easy gig to come by – and I was desperate to keep it. I had been following the research chimp story for a while, and I liked that the N.I.H. chose me to break your news.
I’ve long appreciated how the N.I.H. helps the world. My career began there in 1998, when Paul van Nevel hired me for a science writing fellowship at the National Cancer Institute. I count your communications director John Burklow among my mentors, and I was honored to write Paul’s obituary. That first boost of professional success propelled me to an exciting career.

Lately, though, my love for your august institution has been strained. You see, I’ve been felled by the most forlorn of orphan illnesses. The most accurate name for it is myalgic encephalomyelitis, which means “painful inflammation of the brain and spine.” (Yes, it is painful, and yes, there’s strong evidence of neuroinflammation.) At the N.I.H. and elsewhere, it is instead called chronic fatigue syndrome. That’s a terribly vague and dismissive moniker for so serious an illness, and one that needs to be retired. Fatigue is not the primary or most troubling symptom for most people with M.E.
In the past, you’ve shown a soft spot for certain orphan diseases. Well, the history of M.E. is akin to locking an entire orphanage in a cellar and bulldozing the house.
On the list of illnesses the N.I.H. studies, M.E. (listed as “M.E./C.F.S.”) is near the bottom in funding, ranked 231 out of 244. It received $5 million in 2014, less than hay fever, which cripples no one. That’s not enough money to equip a laboratory and run it for a year. This abject neglect – or sustained prejudice, or maybe both – stretches back a full three decades at the N.I.H. (For a detailed history of how this sad state came to be, read Hillary Johnson’s deeply-reported book Osler’s Web.)
No one has a good count of M.E. patients in the U.S. – the C.D.C. misspent funds earmarked for this purpose – but there’s plausible evidence that several hundred thousand people are disabled by it. That’s comparable to the burden of multiple sclerosis – the illness M.E. most closely resembles. N.I.H. funds $110 million in M.S. research each year, and a sustained government investment has been crucial in the development of a dozen F.D.A.-approved M.S. drugs. M.E. patients have no approved treatments.
But M.E. is finally emerging from the basement. Brand name institutions and big-time researchers now recognize the huge burden M.E. places on society – tens of billions in medical expenses, lost productivity, and missing tax revenue each year. Columbia University’s Ian Lipkin is searching for infectious triggers, and has reported severe immune problems in patients. Columbia received $150 million in N.I.H. grants in 2015; Lipkin’s operation gets a big chunk of that. But when the famous virus hunter applied for a trifling $1 million for M.E. research, the N.I.H. turned him down, twice. So spurned, Lipkin and colleague Mady Hornig recently resorted to eating habanero peppers to raise money.
Jarred Younger, at the University of Alabama-Birmingham, has a list of off-the-shelf drugs and supplements that can reduce neuroinflammation. They urgently need to be tested in patients. In Norway, a phase three clinical trial of the cancer drug Rituximab in M.E. holds great promise. In early trials, nearly two-thirds of patients improved after repeated doses of Rituximab, and a quarter went into full remission. Such promising results, if reported in cancer patients, would be trumpeted as a breakthrough. Additional studies to sort out which patients might benefit from this drug are urgently needed; the N.I.H Clinical Center would be a fantastic home for such trials. It’s unseemly to let a tiny Scandinavian country overtake the enormous U.S. of A. in this, or any, realm of medical research.
At Stanford University, prominent geneticist Ron Davis is searching for genetic risk factors. His investment is deeply personal, as his adult son – formerly a world-traveling photographer – is severely ill with M.E., and can no longer walk or talk.
When you peruse the recent M.E. literature, you’ll see a mix of young researchers and experienced lab leaders producing a string of insights into how the illness damages the immune system and the brain. Mutations in the gene MTHFR have been identified by the Open Medicine Foundation as a risk factor. Diagnostic biomarkers await validation. Promising treatments need to be tested in patients. And all of this has happened with little support from the N.I.H.

Patient advocates have called for $250 million in M.E. research funding, a figure commensurate with the burden of disease. This is a huge ask, and in all likelihood politically infeasible, so let me make a smaller one. A new N.I.H. program funded with as little as $10 million to $20 million per year would be absolutely transformative for the field – and for patients. Such a program would affirm the N.I.H.’s commitment to understanding the illness. It would draw more young researchers to studying M.E., and it would encourage further private funding. Such a commitment would also give patients – many housebound or bedbound for decades – hope that they’ll be healthy again. I challenge you to find another illness where such a small investment could make such a huge difference.
You now have broad support from the medical community to make this happen. Earlier this year, the Institute of Medicine made a strong call for a robust M.E. research program. And just last month, an N.I.H.-appointed panel urgently made the same recommendation. With the bipartisan 21st Century Cures Act poised to pass Congress – giving N.I.H. an extra $8.75 billion over five years – you could do so without pulling money from existing programs. At the same time, you could help things along by moving responsibility for M.E. from its long-term parking spot at the Office of Research on Women’s Health to one of the institutes that, you know, funds disease research.
A year before I fell ill, I backpacked Rocky Mountain National Park. My legs carried me up to the continental divide, where I sat on the edge of a precipice marveling at the peaks around me. At nearly 13,000 feet above sea level, the thin air addled my thinking – a feeling I now live with every moment, as if someone poured molasses into my ear, gumming up all trillion synapses. It’s a terrible way to go through life, especially so for someone who not so long ago made a good living with his brain.
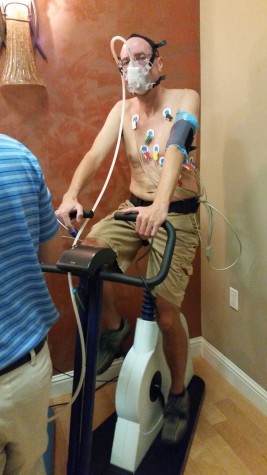
Here in Hawaii, there’s a smaller mountain behind my yard. It’s called Sleeping Giant, and the giant’s forehead juts less than 500 feet above my back patio. A well-trod trail carries people up there for sweeping views down the volcanic slope and across the endless Pacific. Oh how I would love to drink in that view. But I may as well be gazing up at K2; a summit attempt would be supremely unwise, as a sophisticated exercise test found that I suffer from severe metabolic, cardiac, and pulmonary dysfunction. Exercise for M.E. patients is more damaging than sugar is to a person with diabetes.
At 43, my productive life may well be over. There’s a good chance I have hiked my last trail. The nation’s coffers lose some $25,000 in tax revenue each year I remain disabled, and I will soon know if Social Security Disability Insurance will start coming my way. I don’t enjoy being a drain on society, and neither do any of the other M.E. patients I know. And yet, with the ever-growing research interest in M.E., I have hope that someday I’ll be able to stand for more than a few minutes, walk for more than a block or two, maybe even resume my career. (It took me four days, with frequent breaks, to write this letter…that’s a bit slow for newspaper work.)
The causes of M.E. will eventually be discovered, treatments will be found, and patients will enjoy long-term remissions. As the leader of our nation’s medical research enterprise, you have a decision to make – do you want the N.I.H. to be part of these solutions, or will the nation’s medical research agency continue to be part of the problem? At the very least, you could ensure Dr. Lipkin doesn’t have to scorch his intestinal tract again just to drum up a few research dollars.
Sincerely,
Brian Vastag
This is superb, Brian. An absolutely superb piece of advocacy. I hope that Director Collins can hear you.
You’re right: $250 million would put us on a per-patient par with similarly disabling diseases, but just $10m or $20m would be transformative. We have the world-beating scientists such as Ian Lipkin and Ron Davis ready to go as soon as they have the money.
It’s disgraceful that they have to struggle to raise money bit by bit from patients — patients who are so sick and disabled that we’re mostly broke and unable to fundraise.
It’s time for the NIH to do as you ask: fund this research, and move this disease out of Women’s Health where it can get proper funding. It’s not a ‘women’s disease’.
Thanks, Brian. I am a friend of Beth’s.
My only quarrel with your letter is this: don’t sell us short. We deserve to be funded at the same per capita as diabetes or HIV. It is currently far easier to manage either of those diseases than ME/CFS/SEID. I request you be bold, sir. Ignore the political realities and ask for what is true.
Thanks, Brian, for a brilliant letter. I hope Francis Collins takes your words to heart.
I agree that $250m is the right kind of figure for research to match the scale of the suffering and economic cost. I also agree that $20m would make a huge difference to the field, and surely can’t be too hard to deliver. It would be a great start, and a sign that the NIH is beginning to get serious about ME/CFS.
Brilliant letter. Thank you! Sharing now. xx
Thank You
very good letter, thanks for using your limited energy to write it.
have had cfs/me/SEID over 27 yrs, most I’d my adult life, and admit I have lost hope of leading a normal life in this system . but really any improvement would help. I really hope someone , anyone, with clout listens to your letter and gives us at least a steady dribble of funding as you requested rather than the pitiful less than a drop we get now
Brian, so sorry to hear of these struggles! Very eloquently written. I have learned much from what you said. I can understand your frustrations with a debilitating illness. I have struggled for four years with cancer all over my bones and now a messed up thyroid from medical interventions causing chronic fatigue. Definitely not a fatigue that should be lumped into the same as yours but it is so hard to function daily. I was recently hospitalized for a tumor pressing into my spine causing paralysis. How I had to independently get myself up the stairs to my apartment was just as you described. So much “cancer awareness” and “cancer research” is a joke to me. Spend all they want, but there’s nothing they can do to help me, only further destroy me with treatments. I do hope your advocacy gets the attention you and others with ME deserves. For me, I will trust in the Lord. I pray also for you. I have so much respect for you after reading this. I believe we went to school together…maybe you were a year ahead. (Southwest ’90)
As a minor note, while hay fever may not cripple me, it sure has a significant effect on my productivity and quality of life. It’s another form of aut0-immune disorder, which seems like one of the huge areas of medical ignorance at this time.
Best of luck to you, Brian.
Just ‘thankyou’! I hope Collins reads this with the intent I have done.
Thank you, Brian, for writing such an excellent letter and for advocating from your bed. I strongly encourage Dr. Collins to heed your advice to become a champion for this illness. Presently, I’m being treated for M.E. with the “experimental drug” Ampligen. It blows my mind that of the several hundred thousand M.E. patients in the U.S., only about 30 of us have the privilege (because of location and cost) to take this very helpful M.E. drug (which has remained stuck in the FDA labyrinth for approval for over 20 years). If you want to do your next article or blog on that, feel free to contact me. All my best to you.
brilliant thanks from australia the powers to be are just as hopeless here
Thanks so much. Hoping Dr Collins will show compassion.
Thank you for a very courageous letter! Beautifully written! Am sharing.
Karen – Ah yes, the long, sad Ampligen story. Really a damn shame the FDA rejected it last year. How much is it helping? And did you have sudden onset or gradual?
When negotiating, you always ask for more than you want, as it will often be negotiated downward. If you ask for $250M, you might get $10M. If you ask for $10M, you might get a few hundred thousand. That being said, $250M is not an outrageous number, it only puts M.E. on par with similar diseases.
$250M is mere pocket change for the NIH. If the will was there, the money would be found, just like $2.9Billion is found for AIDS every year. The squeakiest wheel gets the most funding, regardless of the disease burden. Be bold, ask for what you deserve; do not accept crumbs.
Thank you very much for the effort it took to write this excellent appeal for funding from an institute that has neglected and just turned its back on ME patients for so long. I do hope that the tide is turning.
4 days it took you. But You still got it in You! Thank You so much for this incredible effort. I can only hope it touches a nerve in director Collins’s healthy body.
Hi Brian,
I am curious have you ever taken a Fluoroquinolone Antibiotic? Cipro, Levaquin, Avelox, Floxin and there are others. Many of us suffer from the ADR’s like you have described. If you have …please feel free to contact me or join us on FB https://www.facebook.com/groups/191063714251094/
Thank you for your eloquence and for the extended effort, which no doubt had a high personal cost. Your professional skill and courage shine through brightly. Thank you.
I’m so sorry about your illness. Your letter is wonderful and you should be writing without the terrible impediments thrown in your path by this disease. If you come to Boston for medical help, you will always have a place to stay. (bring your mom, my cousin Bonnie.)
Your appeal for more research is eloquent and important. The Fluoroquinolone family of antibiotics including Cipro, Levaquin, and Avelox has similiar devastating life changing side effects that are under-recognized and under reported. These side effects can occur up to a year after you take the antibiotic. I took Levaquin (Levafloxacin) and immediately went from a vibrant, athletic, working woman to being unable to walk, bedridden for most of the day, all of my tendons damaged, and suffering crushing fatigue. If my conditions hadn’t been directly attributed to the side effects of the antibiotic I may have been diagnosed with one of the many autoimmune conditions like CFS. These antibiotics are currently the most prescribed antibiotics world wide. YES more research is needed to understand contributing factors like genetics and adverse drug reactions so that medical solutions for cellular/DNA damage can be developed.
Thanks Brian. I wish you as well as possible.
Brian, be sure you get tested for tick borne diseases. Some cases of CFS are actually Lyme. If so, you MIGHT improve on antibiotics. Can’t hurt to check it out.
Well, a year of rotating antibiotics didn’t seem to help…
If I die before they find a cure for our kids who have been sick for a decade..I am coming back as a kick ass virus hunting , nobel prize winning mitochondrial research wizard..and make these guys wish they had tried harder.
Thank you for exquisitely detailing the daily challenges that so many of us face. Sometimes I feel so frustrated educating friends, family, and health care providers. I can now refer them to your letter so they can better understand my limitations and also the economic impact of delaying research dollars to solve me/cfs. We also need to understand WHY so many people are suffering from chronic diseases (diagnosed, mis-diagnosed, un-diagnosed). We need more research and data so we take steps to toward building a healthy environment, safe Rx’s, and health care that focuses on preventative care. I look forward to reading more from you in the future. I appreciate you! YOU MATTER!
Thank you for your eloquent letter. I seriously hope that your words have some impact on Dr. Collins. This illness – call it ME, CFS, CFIDS or SEID – needs to be a much higher priority item in future NIH budgets.
Just to give one example, with more ME research studies we’d probably have a better handle on diagnostic criteria and subgroups and less confusion over what to call this illness. We’d be focusing on treatments and cures instead of still fighting over the name.
I got sick in 1990 at age 29. With all that’s happened over the years, I’ve almost given up hope that anyone in our government (CDC, NIH, HHS) has any desire to help ME patients. I don’t like feeling that way, but there it is.
People don’t realize how much we want to be well. Not only do I miss the everyday socializing and leisure activities I also really miss working. I would be so much happier to be a tax payer again and be putting into the system instead of taking from it.
And as much as I have enjoyed the #ChilliMedChallenge videos, it is a shame that patients and patient advocates have to resort to crowdsourcing funds for proper biomedical research for ME.
That was a great post. Your writer’s instincts are still inside there. I, too, was a writer – a historian – and lost my rising career at the age of 44. I suffered blackouts, massive confusion, disorientation, ataxia, expressive dysphasia, short-term memory loss (and later learned I had trouble forming memories). For someone who used to read for a living, it was horrible not to be able to read at all – but print looked like cyrillic alphabet to me. I could read a little online so I had friends through internet.
And then there was the pain. For the record, the Myalgic in Myalgic Encephalomyelitis stands for muscle pain. I had what I called my encephalitic pain – intense pain behind my eyes and in the back of my neck, and headaches like migraines but double-sided. But I also suffered from constant muscle pain, particularly in my legs, but also my chest.
I was lucky – my family stayed with me. My daughter was 13 when I collapsed and spent her high school years taking care of her mother – but my husband made sure she stayed in outside activities.
I was also lucky because in late 1997, three years after my collapse, I was diagnosed with HHV-6A, first discovered among AIDS patients, by Dr. Dharam Ablashi, the co-discoverer of HHV-6 and its two variants (HHV-6B is roseola and a different virus entirely). I also tested positive for the 37kDa Rnase-L defect. So I began treatment with Ampligen on 4 Feb 1999. My two biomarkers were gone in six months. I was walking without a cane in two months; could drive again in three; did away with the wheelchair entirely in four; read a book in six; and seven months after starting Ampligen, I did the mother-son dance at my son’s wedding.
I am a fast responder to Ampligen – but, unfortunately, I am also unique in that I cannot stay off it. The first time I went off (I thought I was cured), in October 2000, one year later it all came back. After that, we were determined I would stay on it, and I did, for five years. Then the head of my practice died and FDA took the drug away. There was no place within 100 miles anywhere to get it. within 7 months I had completely relapsed.
I was using Southwest points to go to Tahoe to see Dr. Peterson once a year, and already had an appointment coming up when I collapsed the second time, in 2008. He found I had a natural killer cell function of 2%, the 37kDa Rnase-l defect was back, and I also had an abnormal cytokine pattern. I had abnormal SPECT scans, Halter Monitor tests, and a very abnormal CPET test – so bad that I would be considered a severe cardiac patient and eligible for permanent disability on that score alone.
I was, of course, back in a wheelchair, back with sunglasses all the time because light hurt my eyes, confused, in pain – all the symptoms I listed above. My husband or my daughter went with me to Tahoe, and thank heavens for the wheelchair pushers in airports.
I still could not get Ampligen at home, so we tried the antiviral Vistide, but my liver rejected it. in 2009 Dr. Peterson found I had HHV-6 and CMV active in my spinal fluid. Later I mentioned that to someone high up at CDC – and he said “No, you didn’t. You people test positive for diseases you don’t have” – and walked out of the room.
Now, it seems to me that finding viruses known to be neurotropic active in your spinal fluid just might explain why a person has so many symptoms of encephalitis and meningitis! Not with us, I guess. The cognitive dysfunction at CDC and NIH is just too strong.
I ended up having to move out to Tahoe to get back on Ampligen – and again, I got better fairly quickly, but I missed my husband terribly. When a chance to get it in NYC opened up, I jumped at it. So in 2010-11 I was living away from my husband at Tahoe; in 2011-2014 I commuted 100 miles north by Amtrak twice a week to get Ampligen. It is that necessary to my ability to have a life at all.
My husband died of cancer two years ago – at least I was well enough to be of help to him in his last months, thanks to Ampligen. We were married 40 years, and I will never get over losing him. But I have now moved to Tahoe permanently, where I can get Ampligen a couple of miles from my house. And I have my Irish setters with me now.
Not every ME patient will benefit from Ampligen. But if it was only 10 percent, that would be at least 100,000 people. FDA has admitted in writing that it has no major toxicities – certainly it is tamer than my alternatives, such as Vistide. But FDA does not believe the small one-product company has made its case, and I have been told privately they “don’t deserve to make a profit.” oh yeah, that’s what we should be thinking about. Not patients. Not medical science. Profit.
You need testing. You need a good doctor. They’re out there, though you may have to wait a bit to see one. This is not as mysterious as CDC and NIH make it to be. It’s just unfunded and unpublicized.
CDC has had its “chronic fatigue syndrome” its own way for almost 30 years. And yet – by their own admission – at least 850,000 adults in the US have the disease and remain undiagnosed. What do the poor do? It has not escaped our attention that people of color are not proportionately represented among the diagnosed – so where are they? Lenny Jason showed years ago that this is an equal opportunity disease when it comes to income and ethnicity – not so for diagnosis, and certainly not so for treatment. But you could say it is equal opportunity in terms of impoverishing anyone who gets it, no matter whether they had attained a professional career or not.
This past month we lost several patients, but among them were 2 28-year-olds. One, a surfer, committed suicide. The other, who had been very sick a long time, died of an apparent heart attack in her sleep – the disease just wore out her body.
I ask – just what will it take for NIH and CDC and FDA to do the right thing by us? How many of us have to die? How many of us have to lose everything we thought worth having? And what a waste of human beings.
Thank you for your blog. As my British friends say, it was brilliant.
The letter you wrote is brilliant (you had me at the title!) I could go on and on but it’s really as simple as that. And it’s not brilliant because you are obviously an eloquent writer (which you are) or that you made *so many incredibly gripping points, although you did. ((I too have always marveled hayfever gets more funding than we do. People that “achoo”, rank higher than people that are bedridden – that’s enough to blow anyone’s mind)). But beyond all of that, I think it’s brilliant because you shared *your story & in that, it touches people. As a patient since I was 11, I know it spoke for – and to – me.
I saw Ampligen was mentioned… I had sudden onset. I can actually remember the hour I got sick. I also had 3 other family members that were all there with me at that time, eventually get sick as well.
I am one of the Amp patients in the original 100 patient “compassionate care” trial. Basically they agreed you were so deathly sick you had no choice but to try the drug, but that’s the end of the compassion. After that, you’re on your own to pay the extremely high cost to get the drug (at that time it was ridiculously expensive because you had to take a very high dose and it had to be kept frozen until use, all of which added to the expense).
To make the families of bedridden patients, mortgage their savings, desperate to find any help for their loved one, for a drug that should have been approved & covered by insurance (or sold at a lower cost) years ago… it’s a crime. Especially since there has never been a serious issue (heart attack, stroke, etc) with any patient on Ampligen and for patients like myself – I believe it saved my life.
This is just a brilliant piece of work. Thanks, Brian.
Thank you. Thank you. Thank you. You have given me hope.
Great letter, Brian!
Did you mail or email it to Dr. Collins?
Thank you.
Brian, thank you for your straightforward letter to the NIH. It would be great if they took note. It appears that they prefer to ignore M.E. (or have ‘workshops’ etc. that come up with more denigrating names) than fund it. It’s almost like the powers-that-be collude.
When we think of Dr. Ian Lipkin’s calibre and of his being turned down for a measly $1m research fund, it tells it all. NIH, and the others, do no want to fund anything to do with M.E. This needs to change. We all know that Dr. Lipkin’s funding would not have been turned down had it been any other illness. It was just because it was for M.E.
I am very thankful that Dr. Lipkin et all are persevering on our behalf and that we have people of their intelligence, experience, tenacity and dedication in our corner. They’ll find what needs to be found. But very sad that they had to resort to crowd-funding.
It’s also very hurtful that there is a drug, Ampligen, that seems to help quite a number of people but was not approved by the FDA. Hemispherx, I believe, is now applying elsewhere for approval of this drug. Since I live in Ireland, I suppose it won’t be available in my lifetime. After more than 28 years of M.E., one could say that I’ve seen it all and seen nothing!
However, I fully support and promote the #chilliMEchallenge. It is biomedical research that will end this torture. So, if anyone here is reading this, please support this challenge. It is our biggest hope. All donations are going directly to biomedical research.
Governments worldwide are not fighting for us. It is my opinion that what has been done to people with M.E. will go down in history alongside the other abuses perpetrated against people by governments and their agencies.
Many thanks for your wonderful letter.
i am so disappointed in dr collins. i thought he was compassionate. i remember reading that he has failed to attend any of the CFS/ME related meetings.i read his book on how faith and science can co-exist but dr collins has shown the same callous indifference to this terrible disease,as his predecessors. if you pay attention to the speech and conduct of nih officials when it comes to this illness, you can see that the next 25 years are going to be like the previous 25-the nih has the capacity to fast track this disease, but i wouldnt hold my breath.
Thank you for the enormous effort you went to, to write this letter. It is incomprehensible why so little research is being done into ME. Research, research, and more research is the answer – and humane, considerate, understanding treatment of ME patients by the medical profession.
Brian, thank you, thank you, thank you for your brilliantly written letter. Having had ME/CFS since 1986, it is sometimes difficult to maintain any hope of returning to whatever my normal life might look like. For whatever reason, your letter revives my spirit and renews my hope. I’m so sorry that you are ill, but so thankful that you are able to speak out so eloquently on behalf of other patients unable to speak for themselves. God bless you Brian.
I’m so sorry to hear you’re dealing with this, Brian. This is a wonderful letter, and I know how challenging it was write. My father was among the first group of patients officially diagnosed with “CFS” in the 80s, when I was sixteen (when it was being referred to as “Yuppie Flu”). He was in the original (ill-fated) ampligen clinical trial (I’ve often said that watching him struggle with his illness and diagnosis, and that clinical trial, is one of the things that turned me into a science writer). I’ve been following all of this to some degree ever since, and have always thought I should write about it someday. As my father has said and written many times: calling this disorder Chronic Fatigue Syndrome is like calling diabetes Chronic Peeing Syndrome, or emphysema Chronic Coughing Syndrome. He’s written several books about his own experiences, including his struggles with learning to write again after brain damage (starting with “The Night Side: Chronic Fatigue and the Illness Experience”). In case you’re interested and haven’t seen them, you can read a few of his essays online: http://www.missourireview.com/archives/bbarticle/wild-in-the-woods-confessions-of-a-demented-man/ And http://www.gettysburgreview.com/selections/past_selections/details.dot?inode=9f014417-4f22-473d-acfc-ee173ce8755b&pageTitle=Floyd%20Skloot&crumbTitle=Trivia%20Tea:%20Baseball%20as%20Balm&author=Floyd%20Skloot&story=true. Wishing you all the best.
Thank you Rebecca. Your father’s essay in the Times last year (the year before?) made a big impression on me. And seeing that he’s written several well-reviewed books while ill gives me hope I’ll be able to continue my career in some fashion. So tell him thanks for me.
Brian, thank you so much for your wonderful letter. I have been ill since Jan. 26, 1985 when I had a sudden onset. This devastating illness seems to be making its rounds again, in an outbreak fashion, like polio used to. We desperately need research. We need to stop seeing valuable lives wasted.
Thank you and God bless you.
Howdy folks.
ErikMoldWarrior here.
I am an Incline Village survivor and member of the original CFS cohort.
Approved for ampligen, and all that stuff.
I walked out of the ampligen program to “Try something crazy” instead, and wound up returning to hiking and mountain climbing.
Yes, yes, I know all about the HHV6A, as I am from the very outbreak in which this virus was first detected, as told in Osler’s Web.
Now, it is very interesting that BEFORE Brian got the flu like illness, he was suffering from altitude sickness at 13,000 ft.
I realize that people have come to think of this as being normal for humans.
It isn’t.
It’s a clue that something was wrong.
-Erik Johnson
Oh come on Erik – Someone who lives at sea level getting a little hypoxic at 13,000 feet isn’t normal? Please.
THANK YOU!!!!
Thank you! I truly hope this letter is read by Dr. Collins and that it makes a difference for all of us.
Great letter, Brian! Thanks much for putting the effort into it.
For those asking if Dr. Collins has read the letter – two people who work in his office told me “it’s being passed around” and they flagged it for him to read. I’ve been told to expect a response at some point. We’ll see…
Well said, I hope your letter gets traction with Dr. Collins and his peers.
Thanks for that powerful piece!
Please don’t anyone take this next comment amiss. Francis Collins in all likelihood will never read it. Nor will anyone who can make a difference for us at the NIH. That’s a real shame because this is very powerful piece. The reason for that is that without a group of people dedicated to making a difference for ME/CFS at the federal level we have very little pull there. We’re simply hoping that someone is going to do the right thing. Hopefully they will but we should be clear that’s so long as there is no one walking the halls of Congress, no one producing a strategic approach for getting more money…that’s what we’re relying and what we have relied on for many years. Hopefully someone is doing – it would be a great help.
I loved this comment – heartily agree with it!
“Additional studies to sort out which patients might benefit from this drug are urgently needed; the N.I.H Clinical Center would be a fantastic home for such trials. It’s unseemly to let a tiny Scandinavian country overtake the enormous U.S. of A. in this, or any, realm of medical research.”
and this one”:
“At the same time, you could help things along by moving responsibility for M.E. from its long-term parking spot at the Office of Research on Women’s Health to one of the institutes that, you know, funds disease research.”
and this one:
“Exercise for M.E. patients is more damaging than sugar is to a person with diabetes.”
“The nation’s coffers lose some $25,000 in tax revenue each year I remain disabled, and I will soon know if Social Security Disability Insurance will start coming my way. I don’t enjoy being a drain on society, and neither do any of the other M.E. patients I know. ”
You have got the touch. I hope you keep writing 🙂
Having just passed my 21st sickiversary, I appreciate this excellent letter.
I encourage people to paste the full text of this blog into an email sent to Collins and cc’d to other powerful figures. Here are addresses:
TO: francis.collins@nih.gov, collinsf@od.nih.gov
CC: Sylvia.Burwell@hhs.gov, Tomfrieden@cdc.gov, eunger@cdc.gov,
AND your 3 congressional representatives
Well, the good Dr. Collins did read my letter and sent me a response an hour ago. He asked me to keep it private, which is fair. But I will say that his words conveyed to me that he does understand how serious the illness can be, and he made a pledge that gives me cautious hope that change may be afoot at NIH. We’ll see…